A selfie might save your life. The camera on your phone could be used to test for cervical cancer and HPV, a virus that can lead to the disease.
Diagnosing disease is costly and time-consuming, especially in countries with limited resources. Ralph Weissleder of Massachusetts General Hospital, Boston, reckons digital holography – the construction of 3D images of cells using a smartphone-compatible device – could help.
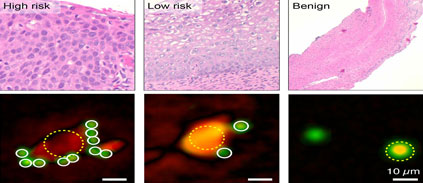
To turn holography into a diagnostic tool, Weissleder’s team first had to make different molecules, such as those collected during a smear or pap test, diffract light differently. They did this by adding microbeads, which bind to specific molecules – such as cancer markers or HPV DNA – and change their diffraction pattern.
They then inserted the sample into a device that clips onto any smartphone. Light is shone onto the sample and patterns of diffracted light are detected by the phone’s camera. The more microbeads visible, the greater the risk of cervical cancer. These are sent to a computer that reconstructs an image of the cells present. This image is sent back to the phone, along with the result. The process costs $1.80 and takes 45 minutes.
The device was able to distinguish between women who were at high or low risk of cervical cancer and to detect the presence of HPV as accurately as conventional tests.
The team also tested microbeads that bind to markers associated with blood cancer. In a pilot trial, the microbeads were tested on samples of lymph, the fluid that circulates around our lymphatic system, taken from people with enlarged lymph nodes. This can be a sign of infection, or the presence of benign or malignant tumours. The smartphone analysis confirmed the presence of cancer cells in four people, and excluded the diagnosis in another four, matching the results of conventional tests.
Weissleder is now planning on piggybacking on an HIV project in Botswana to test the device’s ability to detect cancers exacerbated by HIV.
There are fewer than 10 pathologists in the whole of Botswana, says team member Cesar Castro, also at Massachusetts General Hospital. “They don’t have many chemotherapies available so there’s an opportunity to make a real difference – we can use our technology as a kind of triage system, to flag up samples that look suspicious and help put resources to the best use.”
While people in low-income countries might benefit the most from smartphone diagnosis, future iterations of the device that detect diffraction patterns in a spot of blood from a pricked finger could enable people to diagnose themselves at home, says Castro. Tweaking the structure of the microbeads should mean infectious diseases and other types of cancer could be picked up. “The user would get an image and an analysis of the results that could be sent to their doctor,” he says.
NewScientist

